
Family Dentistry Services by Morris Family Dentistry
At Morris Family Dentistry we are dedicated to providing oral care services to individuals of all ages, from children to adults. We focus on preventive dental care, regular check-ups, and treatments to maintain healthy teeth and gums for the whole family. Our dentists are trained to identify and treat various dental issues, such as cavities, gum disease, and tooth decay, and provide advice on oral hygiene, nutrition, and lifestyle habits that can affect oral health.
Our services typically include routine dental check-ups, cleanings, fillings, and fluoride treatments, as well as more complex treatments like root canal therapy, extractions, and orthodontic services. With a focus on providing comprehensive care, our family dentistry services are designed to meet the unique oral health needs of each family member and ensure a lifetime of healthy smiles.
Call us Now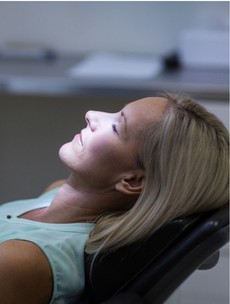
Bite Guards for TMJ / TMD

Emergency Dental Services

Dental Implants

Sedation Dentistry

Wisdom Teeth Removal
Bite Guards for TMJ / TMD
A bite guard is made of plastic and snaps onto the teeth (in this photo the upper teeth). It is the treatment of choice for excessive tooth wear, pain in the temporomandibular joint (TMJ), pain in the jaw muscles, or pain in the teeth caused by grinding or clenching. The bite guard is usually worn while sleeping because grinding is most common during sleep. It may also be worn during the day if grinding or clenching are daytime habits.
Why Does a Bite Guard Work?
It limits wear and tear of the teeth. Even if you grind and wear out the bite guard it is better to wear out the plastic that can be replaced rather than your own teeth. When you grind or clench in your sleep the pressure on the teeth is many times greater than normal chewing forces when eating.
The bite guard also keeps the teeth apart or open a few millimeters when compared to the natural bite without the bite guard. This slightly-open position stretches the jaw muscles to a weaker position, so even if you continue to grind or clench is done with lower forces.
These weaker forces are will reduce or eliminate pain in the jaws and teeth.
Furthermore, bite guard is flat. The lower teeth will skate smoothly along the bite guard. This also reduces the force of any grinding when compared to grinding on the teeth that interlock. Teeth without a bite guard that fully interlock suffer during grinding due to side-to-side forces on the teeth. Grinding on the smooth surface of the bite guard eliminates these damaging side-to-side forces.

Dental Implants
Every year we help hundreds of patients restore their smile, prevent bone loss, and make eating and speaking easier with the aid of affordable dental implants.
More About Dental ImplantsEmergency Dental Services
When a tooth gets bumped out of position, immediate treatment is required to ensure its long-term health.
Right Away
- Do your best to push the tooth back into the proper position.
- If the tooth has been knocked out completely, hold it by the white enamel end (not the yellow root end), rinse it gently with water only, (do not wipe it or scrub it). Rinse the tooth socket with water, and place the tooth back in the socket, as close to the proper position as possible.
- Call your dentist immediately. If the tooth is repositioned and stabilized in one hour or less, it has a much better chance of healing well and staying alive. If it takes longer than an hour, then it runs the risk of the body rejecting it as if it’s an extracted tooth.
- If the tooth has been knocked out completely and you can’t get it back in the socket, store the tooth in: a. Hank’s Balanced Salt Solution or Save-A-Tooth (available at pharmacies) b. Cool milk c. 0.9% saline water (available at pharmacies) d. Saliva. Have the person whose tooth was knocked out hold it inside their cheek. All these solutions have the purpose of keeping the cells of the tooth alive until it can be placed back in the socket.
If the Tooth Has Been Knocked Out
When a tooth has been knocked out of place there are three areas that might be injured: the nerve inside the tooth, the ligament that secures the tooth root to the tooth socket, or the bone surrounding the tooth. Immediately repositioning the tooth gives the ligament the best chance at survival. If the ligament dies, the tooth may become fused to the bone, or the tooth may fall out completely. If the nerve is injured the tooth may need a root canal within a few days after the injury or even years later.
Baby teeth do not heal well if stabilized because they do not have enough root. If a baby tooth gets bumped, contact your dentist with any questions about what is best for your child.
Treatment for a dental injury to permanent teeth includes repositioning the tooth, stabilizing it, prescription medication, and evaluating the health of the nerve.

Sedation Dentistry
More than half of Americans delay seeking dental care due to anxiety. Delay in dental care may be the difference between a small filling and a root canal or extraction. The need for sedation dentistry to reduce anxiety is undeniable. In our dental practice, we offer three forms of sedation dentistry: oral, nitrous oxide, and IV sedation. Each offers a different level of sedation and relaxation.
More About Sedation DentistryOral Sedation
Oral sedation is a prescription tablet that you take at home before coming to your dental appointment. Most commonly we prescribe Halcion, a sedative. This medication causes drowsiness and amnesia. When you take Halcion you must have someone else drive you to your appointment and drive you home afterwards. Patients who have taken Halcion report feeling relaxed or forgetting parts of their appointment. While some patients sleep through their appointment others will be comfortably relaxed. The medication will wear off within one to two hours after your appointment.
Nitrous Oxide
Nitrous oxide, or laughing gas, causes mild anesthesia and reduces anxiety. It is always combined with 30 percent or more of O2 to ensure safe oxygenation. Patients report feeling heavy or relaxed and sounds seeming muffled. At the end of the appointment nitrous oxide quickly leaves the lungs while the 100% oxygen is given, before you leave the dental chair.
Intravenous Sedation (IV Sedation)
Intravenous sedation (IV sedation) is the most effective form of sedation. Medications are given with sterile water into a vein and have rapid effect. Patients report feeling that just a few minutes have passed and being surprised that the appointment is already over. You will need someone else to drive you home. Medications wear off in about an hour, though it is recommended not to drive or to operate a hazardous device for 24 hours afterward.
Dr. Morris completed his IV sedation training at Duquesne University in Pittsburgh, PA. He is certified by the state of Colorado to perform sedation.
Different sedation options may be used in combination. You may be prescribed oral sedation before coming to the office, then also receive nitrous or IV sedation once you arrive. The purpose of sedation is to eliminate fear or anxiety about dental treatment. It is a comfortable way to get dental treatment done.
Wisdom Teeth Removal
It’s almost a rite of passage, most people will need to have their wisdom teeth removed at some point in their lives. Dr. Morris has helped thousands of teens and adults through the process as painlessly as possible. Read more about these services (and our Internet pricing specials!) on our dedicated web page.
Call us now
For Dental Implant services, call 303-795-1443 today for an appointment!
Call us at (303) 795 1443
Frequently Asked Questions
Everyone responds differently to sedation medications. Some patients sleep while others remain conscious and relaxed. You will be given enough medication to ensure your comfort: anxiety will be gone, and you will have amnesia about some or all of your appointment. While sedated you will be able to talk to your dentist and answer questions, though you may not remember this.
